Risk factors associated with hospital-acquired pneumonia: a literature review
Milton Gerardo Gamboa-Aispuro1 and Fidel Osuna-Burgos2*
*Unidad Médica de Alta Especialidad, Hospital de Especialidades No. 2 del Instituto Mexicano del Seguro Social, Av. Hidalgo, 85120 Ciudad. Obregón, Sonora.
Abstract
Introduction: Hospital-acquired pneumonia (HAP) is one of the main healthcare-associated infections (HAIs), significantly impacting morbidity, mortality, and operating costs of the healthcare system.Objetive: Identify and synthesize the determining risk factors for the development of NIH and ventilator-associated pneumonia (VAP) according to the scientific evidence published between 2021 and 2026.
Materials and methods: A systematic literature review was conducted in PubMed and SciELO using DeCS/MeSH descriptors and Boolean operators. Original studies and meta-analyses in adult populations were selected.
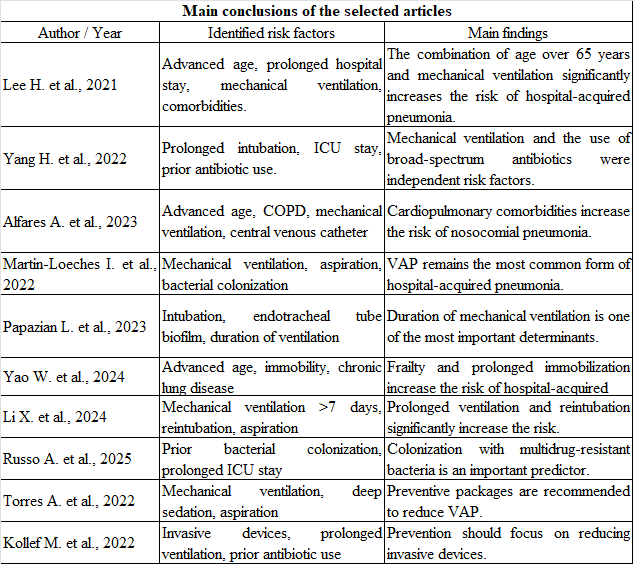
Results: Three risk dimensions were identified: intrinsic host factors (age >65 years, chronic comorbidities), diagnostic-therapeutic interventions (mechanical ventilation, reintubation, previous use of antibiotics) and hospital environment factors (prolonged stay in ICU).
Conclusions: Invasive mechanical ventilation and the frailty of critically ill patients constitute the core risk factors. Early stratification of these factors is imperative for the implementation of prevention bundles.
Keywords: Hospital-acquired pneumonia; Nosocomial pneumonia; Risk factors; Mechanical ventilation; Hospital-acquired infection.
INTRODUCTION
Hospital-acquired pneumonia (HAP), also known as nosocomial pneumonia, is an infection of the lung parenchyma that develops 48 hours or more after hospital admission, without evidence of infection at the time of admission. This condition is one of the most frequent healthcare-associated infections and is associated with increased morbidity and mortality, prolonged hospital stays, and greater healthcare resource utilization.
Within this group, ventilator-associated pneumonia (VAP) is the most severe and frequent form in intensive care units (ICUs). Several recent studies have demonstrated that multiple factors related to the patient, medical interventions, and the hospital environment influence its development.
Objective: To conduct a literature review of recent scientific literature (2021–2026) available in PubMed and SciELO, to identify the main risk factors associated with the development of hospital-acquired pneumonia in hospitalized patients, particularly in intensive care units.
MATERIALS AND METHODS
An electronic search was conducted in the PubMed and SciELO databases using the following keywords: “hospital-acquired pneumonia,” “nosocomial pneumonia,” “ventilator-associated pneumonia,” “risk factors,” “hospital-acquired pneumonia,” and “risk factors.” These keywords were combined using Boolean operators AND/OR. For example: (“hospital-acquired pneumonia” OR “nosocomial pneumonia”) AND (“risk factors”) AND (2021:2026).
The selection criteria were as follows:
Inclusion criteria:
• Articles published between 2021 and 2026.
• Original studies, systematic reviews, or meta-analyses.
• Studies in hospitalized adults.
• Studies analyzing risk factors for hospital-acquired or ventilator-associated pneumonia.
Exclusion criteria:
• Studies published before 2021.
• Pediatric articles.
• Case reports or small series.
• Studies without risk factor analysis. The titles and abstracts of the identified articles were reviewed. Subsequently, those that met the established criteria were selected, and the full text was analyzed to extract relevant data.
The selected articles were evaluated considering the type of study design, sample size, statistical analysis, and control for confounding variables. The included studies primarily consisted of prospective cohorts, retrospective studies, systematic reviews, and meta-analyses.
The results of the articles were compared considering the consistency of the identified risk factors, the magnitude of association (Odds Ratio or Risk Ratio), and the heterogeneity among hospital populations.
RESULTS AND DISCUSSION
Intrinsic Host Factors (Biological Determinants)
Current evidence confirms that immunosenescence in patients over 65 years of age is an independent predictor of NIH (Lee et al., 2021). The loss of protective airway reflexes and altered oropharyngeal colonization facilitate microaspiration. Likewise, the presence of comorbidities such as diabetes mellitus, chronic kidney disease (CKD), and COPD creates a pro-inflammatory pulmonary microenvironment and a deficient immune response, increasing susceptibility to opportunistic pathogens (Alfares et al., 2023).
Factors Related to Medical Interventions
Invasive mechanical ventilation (IMV) remains the most critical modifiable risk factor. The presence of the endotracheal tube eliminates the natural barrier of the glottis, facilitates the formation of bacterial biofilm, and serves as a conduit for the aspiration of contaminated secretions.
• Reintubation and Prolonged Mechanical Ventilation: Recent studies (Li et al., 2024) suggest that the risk increases exponentially after the seventh day of ventilation.
• Selective Antibiotic Pressure: Indiscriminate antibiotic use prior to NIH is associated with a significantly higher risk of carbapenem-resistant Pseudomonas aeruginosa and Acinetobacter baumannii infections (Russo et al., 2025).
Environmental Factors and Clinical Management
Prolonged stays in critical care areas (ICUs) increase exposure to highly virulent nosocomial flora. Other devices, such as nasogastric tubes, alter gastric pH and promote gastroesophageal reflux, favoring retrograde bacterial migration into the bronchial tree.
conclusion
Hospital-acquired pneumonia remains one of the healthcare-associated infections with the greatest impact on hospital morbidity and mortality.
Recent scientific evidence shows that its development is influenced by multiple risk factors, including prolonged mechanical ventilation, endotracheal intubation, advanced age, comorbidities (diabetes, COPD, chronic kidney disease), prolonged hospital stay, prior antibiotic use, and the presence of invasive devices, among others.
Early identification of patients with these risk factors is essential for implementing prevention strategies, such as infection control programs, safe mechanical ventilation protocols, and hospital epidemiological surveillance.
1Licenciado en medicina general por la Universidad Autónoma de Sinaloa, residente de segundo año de epidemiología IMSS UMAE Hospital de Especialidades #2 “Lic. Luis Donaldo Colosio Murrieta” Ciudad Obregón, Sonora. 2 Licenciado en medicina general por la Universidad Autónoma de Durango campus Los Mochis, residente de segundo año de epidemiología IMSS UMAE Hospital de Especialidades #2 “Lic. Luis Donaldo Colosio Murrieta” Ciudad Obregón, Sonora.
REFERENCES
1.Lee H, et al. Comprehensive risk assessment for hospital-acquired pneumonia: sociodemographic, clinical, and hospital environmental factors associated with incidence of HAP. J Hosp Infect. 2021.
2.Yang H, Fan Y, Li C, et al. A retrospective study on risk factors and disease burden for hospital-acquired pneumonia caused by multidrug-resistant bacteria in patients with intracranial hemorrhage. Neurological Sciences. 2022.
3.Alfares A, et al. Risk factors of hospital-acquired pneumonia among hospitalized patients with cardiac diseases. Cureus. 2023.
4.Yao W, Sun X, Tang W, et al. Risk factors for hospital-acquired pneumonia in hip fracture patients: systematic review and meta-analysis. BMC Musculoskeletal Disorders. 2024.
5.Li X, et al. Incidence and risk factors of ventilator-associated pneumonia in intensive care units: systematic review and meta-analysis. Respiratory Research. 2024.
6.Russo A, Serapide F, Alessandri F, et al. Risk factors for development of hospital-acquired pneumonia in patients with carbapenem-resistant Acinetobacter baumannii colonization. European Journal of Clinical Microbiology & Infectious Diseases. 2025.
7.Torres A, Niederman MS, Chastre J, et al. International ERS/ESICM/ESCMID/ALAT guidelines for the management of hospital-acquired pneumonia and ventilator-associated pneumonia. European Respiratory Journal. 2022.
8.Papazian L, Klompas M, Luyt CE. Ventilator-associated pneumonia in adults: a narrative review. Intensive Care Medicine. 2023.
9.Martin-Loeches I, et al. Nosocomial pneumonia: epidemiology, risk factors and outcomes. Lancet Respiratory Medicine. 2022.
10.Kollef MH, Torres A, Shorr AF. Epidemiology and outcomes of hospital-acquired pneumonia and ventilator-associated pneumonia. Clinical Chest Medicine. 2022.
11.Kalil AC, et al. Management of adults with hospital-acquired and ventilator-associated pneumonia. Clinical Infectious Diseases. 2021.
12.Chalmers JD, et al. Healthcare-associated pneumonia and nosocomial pneumonia: current concepts. European Respiratory Review. 2023.
13.Esperatti M, et al. Ventilator-associated pneumonia in intensive care: risk factors and prevention strategies. Critical Care. 2024.
14.Magill SS, et al. Changes in prevalence of healthcare-associated infections in U.S. hospitals. New England Journal of Medicine. 2023.
15.Klompas M. Prevention of ventilator-associated pneumonia. UpToDate/Chest Medicine Review. 2024.
16.Hunter JD. Ventilator associated pneumonia. BMJ. 2022.
17.Torres A, Niederman MS. Ventilator-associated pneumonia: evolving definitions and management. Lancet. 2024.
Citation
: Gamboa-Aispuro GM and Osuna-Burgos F, Risk factors associated with hospital-acquired pneumonia: a literature review, ERSJ 2026,1(4) 247-251